A vasectomy is one of the most effective forms of permanent birth control available – more than 99% effective, low-risk, and far less invasive than a tubal ligation. For men in Brooklyn and the surrounding New York boroughs who have decided their family is complete, the main barrier between making that decision and acting on it is usually a lack of clear information about what the experience actually involves. Lazare Urology performs vasectomies in an in-office operating room under sedation rather than local anesthesia, which changes the procedure experience significantly and is one of the reasons many Brooklyn men choose this practice over others. This post walks through what the process looks like from the consultation through recovery and the follow-up that confirms the procedure worked.
Why Men Choose Vasectomy
The decision is typically a practical one. When a couple has decided they don’t want more children, vasectomy offers a permanent solution without the ongoing cost, inconvenience, or hormonal effects of other contraceptive methods. Compared to tubal ligation, vasectomy is a simpler outpatient procedure with a shorter recovery, lower complication rate, and lower overall cost.
Some men delay the decision for years based on concerns that turn out not to be supported by the evidence. Vasectomy does not affect testosterone levels, sex drive, erectile function, or the sensation of orgasm. The only change is that sperm is no longer present in the ejaculate. The ejaculate itself looks and feels the same – sperm makes up less than 5% of semen volume, and the difference is not perceptible. These concerns are worth addressing directly because they’re among the most common reasons men research the procedure but don’t follow through.
The Sedation Difference: Why It Matters for This Procedure
Most vasectomies performed at standard urology offices use local anesthesia. That means injections directly into the scrotal tissue and around the vas deferens before the procedure begins. For many men, the anticipation of that injection – and the discomfort associated with it – is a significant anxiety driver and a meaningful part of what makes the experience unpleasant.
Lazare Urology performs vasectomies in a certified in-office operating room staffed by both Dr. Lazare and a board-certified anesthesiologist. The patient receives IV sedation – sometimes described as twilight anesthesia – before any local anesthetic is administered. By the time anything happens in the procedure area, the patient is sedated and unaware. The local anesthetic is still used to ensure comfort after the procedure, but the experience of the injection itself is eliminated.
This isn’t a minor distinction. Men who have had vasectomies under local anesthesia at other practices often describe the anticipatory anxiety and the injection experience as worse than the procedure itself. For men in Brooklyn who have been putting off scheduling because they’re apprehensive about the experience, this approach directly addresses that barrier.
What the Procedure Involves
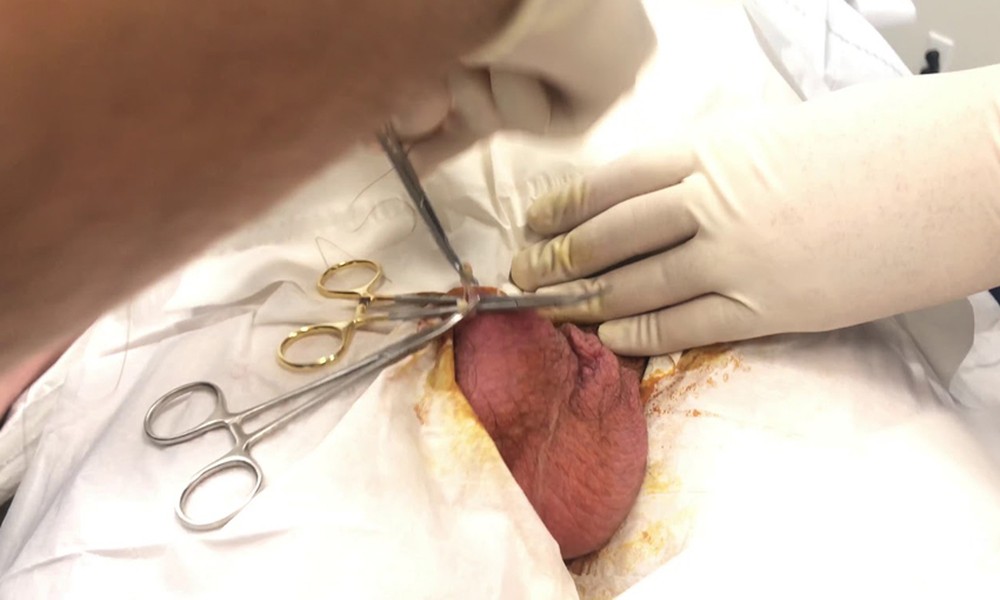
A vasectomy at Lazare Urology takes approximately 20 minutes. The procedure involves accessing the vas deferens – the tube that carries sperm from the testicles toward the urethra – through a small opening in the scrotum. A segment of each vas deferens is removed, and the ends are sealed to prevent sperm from passing through.
The no-scalpel vasectomy technique, which Dr. Lazare uses, involves a small puncture rather than a traditional incision. This approach is associated with lower rates of bleeding, infection, and other complications compared to the conventional scalpel method, and it typically requires no stitches. The puncture closes on its own.
The procedure itself – once the patient is sedated and positioned – is brief. Men are awake and oriented shortly after the sedation is reversed, and most leave the office within an hour of arrival.
Recovery: The First 48 Hours and Beyond
Recovery from a vasectomy is generally straightforward. The standard guidance at Lazare Urology is 1-2 days of rest, with most men returning to desk work and light activity within two days. Physical labor, exercise, and sexual activity typically need to wait a bit longer – usually about a week.
The most common post-procedure symptoms are mild swelling, bruising, and a dull ache in the scrotal area for a few days. Wearing supportive underwear and applying ice during the first 24 to 48 hours helps manage both swelling and discomfort. Over-the-counter pain relief is usually sufficient.
Serious complications after vasectomy are uncommon. Post-vasectomy pain syndrome – chronic scrotal pain that persists beyond the expected recovery period – affects a small percentage of men, estimated at less than 2%, and in most cases resolves with conservative management. Hematoma (blood pooling) and infection occur rarely when the no-scalpel technique is used by an experienced surgeon.
Most men who get a vasectomy in New York on a Friday are comfortable enough to be back at a desk job by Monday.
The Follow-Up Semen Analysis: The Step That Confirms It Worked
A vasectomy is not immediately effective. Sperm that were already in the reproductive tract downstream of the blocked vas deferens can remain viable for weeks after the procedure. Using contraception during this period is essential.
The standard approach is a semen analysis at approximately 8-12 weeks post-procedure, or after 20-25 ejaculations, to confirm that sperm are no longer present in the ejaculate. This confirmation is what allows a man to rely on the vasectomy as his sole contraceptive method.
Lazare Urology has an in-house lab, which means the follow-up semen analysis can be performed at the same practice without an additional referral or lab visit. The result is a streamlined experience from procedure through clearance confirmation.
Rare cases of vasectomy failure – reconnection of the vas deferens – occur, but the incidence is very low, approximately 1 in 2,000. The follow-up semen analysis is what catches this before a patient incorrectly assumes protection that doesn’t exist.
What Vasectomy Does Not Change
This deserves direct and clear treatment because the myths persist. After a vasectomy:
Testosterone production continues normally. The testes continue to produce testosterone, and it enters the bloodstream in the same way it did before. There is no hormonal change.
Erectile function is not affected. The nerves and blood vessels responsible for erection are entirely separate from the vas deferens. A vasectomy does not involve them.
The sensation of orgasm and ejaculation remains the same. The absence of sperm in the ejaculate does not change what ejaculation feels or looks like.
Libido is not affected by the procedure. For many couples, the elimination of contraceptive concern has a positive effect on sexual satisfaction – but that’s a psychological effect of the decision, not a physiological consequence of the surgery.
Scheduling a Vasectomy at Lazare Urology in Brooklyn
If you’re in Brooklyn, Manhattan, Queens, or anywhere in the New York area and are considering a vasectomy, the consultation at Lazare Urology is the right first step. Dr. Lazare will review your health history, discuss the procedure in detail, and address any questions before anything is scheduled. The in-office operating room allows vasectomies to be scheduled efficiently without the logistics of a hospital or surgery center.
Contact Lazare Urology to schedule a consultation. The procedure is short, the recovery is measured in days, and the outcome is a permanent solution that more than 500,000 American men choose each year.